Polysomnography in a Patch
July 4, 2017 | Terry Sharrer
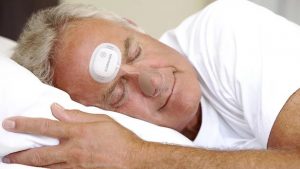
SomnaPatch
Sleep apnea is a risk factor for many serious health conditions. For example, pauses in breathing followed by an abrupt “snort,” inhibit deep sleep which the body needs to restore normal blood pressure and memory processes. Usually, apnea is studied in a sleep lab with multiple electrodes attached to the body, but a new device, “SomnaPatch” (from Somnarus, Mountain View, CA), is worn at night on the forehead, with a connected nosepiece. Sensors in the patch measure nasal pressure, oxygen saturation, heart rate, sleep duration and changes in body position. This piece doesn’t mention the data being wirelessly transmitted, but if it doesn’t it should. Accuracy, compared to conventional polysomnography is high, 87.4% MORE
Image Credit: Somnarus



David W Gerdt
The problem is not using a new technology to detect sleep apnea; a noted sleep doctor told me that many devices are pretty good at detecting apnea at home. The question then is what is the cardio vascular risk associated with the apnea? That is, if a patient has apnea, does CV risk go up or not change much at all or maybe not at all. This is very patient specific information and the routine thing to do is prescribe a CPAP machine, which, when used by a a patient with apnea but without CV risk due to the apnea, can cause more harm than good. The marketing of new devices that can detect apnea at home goes back over several decades and this is one more, but is it useful to a patient or is it hamful if the only action is the prescription of a CPAP machine. The search for CV risk due to apnea will require continuous, noninvasive, beat by beat blood pressure (CNIBP). CNIBP has also been proposed, marketed, and already abandoned for forehead devices. What has been needed for many years is the ability to observe and act on blood pressure spikes due to each apnea event.